Sunday, Mar 13
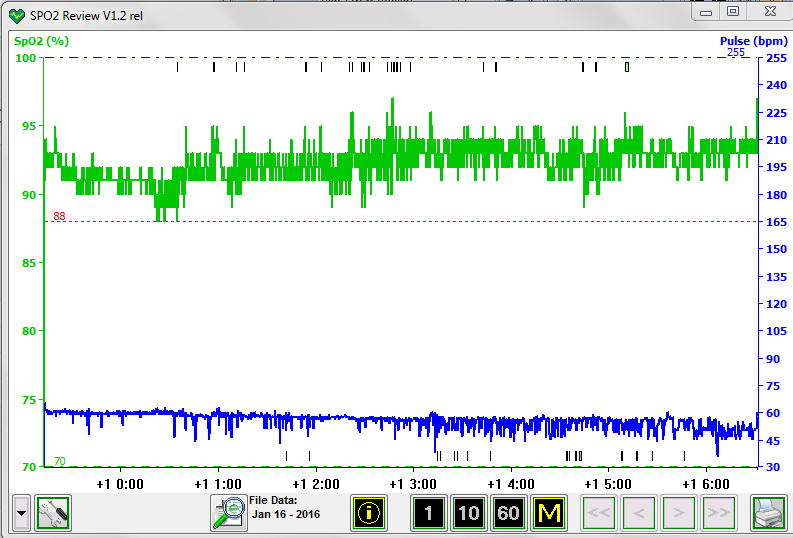
For Mar 12 CPAP. Reported figures, 6 hrs 24 min with AHI=0.94. Events: 6 H, 2 CSR, 15 RERA. No major mask leaks (max=4 L/min); oximeter on entire time with high SpO2 and normal pulse.
I finished my draft of the blog, and John went to town in the old truck to fill with gasoline. While in town, he shopped at Safeway and found a good markdown (50%) on beef stew meat, which he now is combining with beans, onions, and mushrooms into a big Crockpot of chili.
Still need to reset my watch for the day – waited for Daylight Saving Time change.
I have managed to get all my data uploaded from my CPAP and Oximeter. I worked on coordinating upcoming events for our music group, and am sitting watching a wintry mix with about 20% snow now.
Will need to load up my medicines for the week and work on several other projects too. They never end. Trying to set up end of March gigs and get to planning my oral surgery, as well as getting to tax stuff, now that I have the ability to load the Turbo Tax software on my computer where the previous year will carry over.
John saw the sole Ring-Neck Pheasant come in our yard and told me I could get his picture if I’d walk out the driveway some. I lucked out and got a couple minutes of him on video. The wind was wicked and I didn’t have my tripod. We have many quail around but he is the first pheasant I’ve seen in many years. They are pretty birds. Later in the week, Annie had an encounter with him.

This is the same bird in the collage as viewed from each side of his body. To see him in action, follow this link: pheasant video
Monday, Mar 14
For Mar 13 CPAP. Reported figures, 7 hrs 58 min with AHI=0.67. Events: 5 H, 3 CSR, 7 RERA. No major mask leaks (max=10 L/min); oximeter on entire time with high SpO2 and normal pulse.
I went by Karen’s for 2 bags of clothes, on the way to Kathryn’s for sorting clothes for the share, then to the AAC to meet Glenn to transfer some items, to SAIL class, and from there to Burger King for chicken strips and fries (coupon special, $3), a very much needed late lunch at 2:45, having only had a piece of toast early and working hard for a several hours. I only ate half and brought John the rest for his lunch on Wednesday when I’m gone.
I went by the $1 store, looking for St. Patrick’s Day hats. They were out. I drove by Fred Meyers’ parking lot to meet a woman in a Jeep to pick up nice large heavy duty bag with the Costco logo. This was listed free on the BNE site. I have used it much the rest of the week. It is quite large and has long enough strap handles, which I can swing over my back to carry on my right side, but move it to the middle rear for support to be able to carry my heavy violin case with my left arm and balance the bag with my right.

Found out today, where John’s 2 liter bottles went that we mentioned in last week’s blog.
Here is a message from the recipient, “Thank you Nancy. It is for a mini class at Lincoln Elementary where we are going to make recycled rockets with them. They are fun. We fill them with water, pump with air, and they fly up. “Mini science experiment!” [John says: Interesting. One of the possibilities being tried for storing energy is to do this on a really huge scale and then allow the compressed air to flow out and turn an electric generator.]
Tuesday, Mar 15
For Mar 14 CPAP. Reported figures 6 hrs 54 min with AHI=1.30. Events: 5 H, 9 CSR, 11 RERA. No major mask leaks (max=7 L/min); oximeter on entire time with high SpO2 and normal pulse.
Up early to leave before 10:00 a.m. for a 10:55 appointment at the cardiologist in Yakima. We got there and were admitted very close to 11:00 a.m. Justine took all my vitals and gave me an ECG. Dr. Kim came in quickly. He spent a lot of time with us (as usual), but is being cut back on his preferred time with patients by government-induced regulations. He had not seen me alone since last July 14. I had visited with two PAs in the heart center in the meantime after my surgery 12/18. We didn’t leave the building until about 12:45.
We and the staff of the Heart Center are members of Group Health Coop (GH) of Seattle. California’s Kaiser Permanente ($60B annual revenue) is acquiring GH ($3.5B annual revenue). This is supposed to be a great deal for GH but we don’t know if it will be a great deal for us.
From there we went to the Dollar Tree store on Nob Hill Blvd, not too far from the Yakima Heart Center. Needing a different St. Pat’s hat, I had called the $1 store in Yakima, this morning, and got the manager. She checked to see if there were any St. Patrick’s Day hats in stock. She found two and put them at her front register (#1) for me to come check out after my appt. Actually when I got there she had found 5. I picked two and took them. While there, John searched for a new spatula and got a similar silicone spoon as well, both bright red. An ancient spatula’s handle broke on the carrot cake he made earlier. I decided to buy 2 lighting shamrock necklaces too. I gave one of the hats that looks like her daughter’s hat to Amy and gave her the blinking green light shamrock necklace. Daughter Haley called it awesome. I haven’t yet gotten a photo of me in my new St. Patrick’s Day garb yet, but will try before next year, or maybe even put in next week’s blog. We are still doing Irish music, so it won’t hurt to wear it.
On to the foot doctor by way of Burger King. I bought $10 worth using coupons mostly. Got enough for our late lunch and then had leftovers for a late dinner. I got a free Whopper with the purchase of one; $3 worth of 10 chicken nuggets, with large fries, and a small cola. For lunch we halved the whopper (I had the smaller half) and some of the fries and nuggets. We brought home the rest, and added to the leftovers I brought from yesterday for supper. Rather funny as the cardiologist has just told me to lose weight, and he changed the dosage on two of my meds. One is for Uric acid in my kidneys, and John found on the Internet that mushrooms have some chemical that raises a person’s uric acid. Rather concerning as we intake a lot of cooked mushrooms. Bright green veggies are out, so mushrooms have been adding some variety.
Foot doctor. I was scheduled for Laser Treatment of the right foot’s toenails that have had a fungus for awhile. At our last toenail trim (I think we explained this in the blog at that time about DNA testing of toenail clippings), we expected to have a test set up. The goal is to find which other underlying fungi are present that the first treatment did not cure. A medication specific to what’s left to get rid of will be tried; probably a topical one, because I cannot take internal ones that mess with my liver and therefore conflict with my other heart medications. The lab is in Texas so a part of me is now there, or soon will be.
We stopped at Costco for gasoline (good price, $1.95) and picked up a few groceries, including some for our neighbor. We were late arriving back home, about 4:30 p.m. With daylight saving time, John still had light for feeding the animals.
I had to drive back to town shortly after arriving home, to play & sing at the REHAB with The Connections group. It was another long day.
Wednesday, Mar 16
For Mar 13 CPAP. Reported figures 5 hrs 22 min with AHI=0.93. Events: 5 H, 5 CSR, 13 RERA. No major mask leaks (max=5 L/min); oximeter on entire time with high SpO2 and normal pulse.
John took off for his pruning activities before 8:00 a.m.. I only had one cat wanting food – our long-haired small female (fixed) feral kitty, Woody, you have seen previously who comes to a food call to the cable-table 20 feet from the front door.
I started the morning with arranging for an appointment for my Pulmonary Function Test in Ellensburg at our hospital. I have to have it annually to check my lungs because of the Amiodarone I’m taking for atrial fibrillation. The images will show scaring, if any. Thus far, I have had none, being on since March 2010, and have had no reactions to the drug. Many people have problems and have to cease using it. This is good because the alternative requires an overnight or longer hospital stay to set and monitor the dosage.
After doing other paperwork stuff, I drove to pick up Gloria to run around town with me. Luckily, my access to her from the north is in line with the detour around a road I use to get to the northwest part of town the quickest. However, it is closed for water main construction until May 2. We started at the Food Bank, where I was dressed in my new Shamrock hat, but I didn’t get my photo taken either today or on Thursday. Neat that I had invited a BNE person to come by on her lunch hour to pick up a gift from me, and join us for lunch and our singing. She came, got it, and stayed for lunch while we played. We left there with food we transport each Wednesday to our neighbors and went to SAIL (exercise) class at the AAC. We were able to pick up Gloria’s Income Tax forms from the Accountant on our way by. On the return trip, we made a stop for her and us to pick up food items from Grocery Outlet. A few weeks ago we bought 2 cans of Pear halfs there. They were hard and part of the 2nd can got put in a glass jar and slowly found its way to the back of the shelf. Oops!
When John took Ebony her pelleted food and carrots to all the horses he returned with the caution that she was behaving oddly and not interested. A bad sign.
Thursday, Mar 17 Happy St. Patrick’s Day
For Mar 16 CPAP. Reported figures 5 hrs 46 min with AHI=1.21. Events: 10 H, 11 CSR, 13 RERA. No major mask leaks (max=8 L/min); oximeter off entire time, quit working, apparently. (or, perhaps it ran out of battery power).
John left early for a morning of pruning grapevines at White Heron, leaving me to feed the feral cats their morning vittles. Only two arrived in the morning, and the other came back for the evening meal. They have dry food available 24/7.
I started the morning with normal catch up duties, but was sure to pack a bunch of gallon jugs from my neighbor to give to a gal on the BNE site from Thorp. She also needed 18-count egg cartons, which I assembled as well. The plan was to take them by her workplace in Ellensburg on my way home from playing music at Dry Creek/Brookdale assisted living place. I also packed up music and clothes for others I would see there today, and I called in the need for 9 chairs for our play group. We were happy to have our friends from the west side (Winlock) join us to fill the group’s good sound. Dave plays a bass fiddle and his wife Janet plays violin. I’d carried my camera to get some photos of Haley, our mascot, in action as a Leprechaun. I took these pictures before all players arrived. I will describe below the photos.

Haley, daughter of our flute player & tin/penny whistle player, Amy, has on her mom’s made dress and is carrying a pot of gold covered coins (chocolates). Three of the guys are in the background in the second photo, and third shows Amy in her home sewn paneled skirt, with matching green shamrocks material to Haley’s dress. Haley’s hat Amy got at the $1 store in Ellensburg, and I bought the matching hat for Amy at the $1 store in Yakima, Tuesday. On the right is a resident with our sheets of Irish songs for the day. I don’t think she is of Irish heritage, but she has the spirit. Her hat says, “Kiss Me” – “I’m Irish.”

Here we have Haley bringing her pot of gold to share with the players. Left she is with Maury, and right she is handing to Charlie, with Manord and Gerald enjoying in the background, having been previously gifted with candy.
On a sad note, my horse Ebony died last night or while we were gone today, and I came home to find John in the pasture pulling her body with the truck up to the top of our property. He managed to pull her into the hole (previously dug 3 years ago by our friend Allen Aronica with his backhoe), where since then, Shay, Meghan and Dan are resting in peace. Also, there is one neutered feral cat, there. His name was Johnny Cashew (because of his color, and that early in life we called him Little Sue only to find out he was male), hence a man named Sue, a Johnny Cash song. Another neighbor, Ken Swedberg, with a skid-steer** loader, came over and pushed in the rocks and dirt. John is removing some top rocks and rejuvenating the surface.
Link: Explains the name and has a photo
She was near 30, or older – we were told she was 8 when we got here. She could have been older. She’d looked at the hole 3 years ago, and rallied and we’d been supplementing with grain, carrots and apples. She was a talker and would come up to meet us and declare she was ready for dinner. This photo below is the last one I took of her with her special vittles, November 15, 2015, but she seemed in good shape through the winter until just this week.

She was a friendly horse who visited with the neighbors. Last year we were astounded (alarmed and disturbed) to find out cousins of new neighbors’ kids had come through the woods into our pasture (without notifying us) and gotten on her to ride bareback. Happily, she was sweet to put up with it gently.
Ebony was my horse from the 1990s until into the 2000s when she bowed a tendon and could no longer be ridden. She was a cross between a Tennessee Walker and a Quarter horse and had a nice very smooth gait for riding. She carried me around many field trials and on many fun trail rides. I will happily keep those memories.
Friday, Mar 18
For Mar 17 CPAP. Reported figures 7 hrs 16 min with AHI=0.69. Events: 5 H, 2 CSR, 19 RERA. No major mask leaks (max=9 L/min); oximeter on entire time with high SpO2 and normal pulse.
I spoke with a former friend (who knew Ebony) from our old club, Kittitas Valley Trail Riders. Turns out in trying to get information from the Music Library at CWU, I found Mary Wise is now in charge there. She is the one we knew from our past. She led me through the system on line for searching for music, after spending much time searching herself for a song we need in our group, the score for Kingston Trio’s, “The M.T.A..” Access is through cwu.edu and I’m able to login with my “edu” account. I choose Services and then searched All One Search, if not there, then Summit, and finally later in the afternoon she made a document for me with special instructions and emailed them to allow me to search the World Catalog of Libraries (where she had found M.T.A., to get to such things as the Illiad data base, which I can access through the CWU Brooks Library to obtain books through Interlibrary loan on my Emeritus account at CWU. No gold watch, but I do have a CWU parking permit for life and access to the library. Nice benefits for years of hard work and teaching. She had researched and found that only two libraries had the book with the score: one in Texas and one in New York City. Whether they will part with the books for a week is questionable, but I hope they do. I went through the process to request it through CWU. I’m grateful to Mary for the instructions to use in future searches.
Saturday, Mar 19
For Mar 18 CPAP. Reported figures 6 hrs 29 min with AHI=0.31. Events: 2 H, 1 CSR, 11 RERA. No major mask leaks (max=5 L/min); oximeter on entire time with high SpO2 and normal pulse. The extra 1.2 hrs were consistent with higher SpO2 and normal pulse.
Besides working on a card for Ethel’s 98th birthday (John’s cousin in Pennsylvania) coming March 23, I spent all morning sorting clothes from as far back in our history to Iowa (and we came to the PNW in 1974, so that goes way back.) I’m sure there are more packed away. One piece today was a vest-like sweater we both liked, but now it won’t fit us. It was from the Amana Woolen Mill in the Amana Colonies, in Iowa.
Off to town by way of Kathryn’s to drop off 7 bags of sorted clothes: coats, sweaters, men’s Large, women’s L, some XL I don’t need, and 2X. We now have more clothing that we need. I still have 3 days left until the clothing share on Tuesday to sort out more to get to good homes and clean up our clutter.
While moving stuff from my car to John’s, so I could drive it and get him some gasoline and cased-sausage (summer or non-refrigeration type) for his last day of pruning, I realized I had left my Irish music in my tote bag container on a table in the dining room, at Dry Creek, on Thursday. It would have been nice if someone on the staff had notified me, but they didn’t. I called on my way into town and asked if it had been turned in. The only one woman at the front desk was busy and did not have keys to the business office, where it might have been left. I described the bright green bag it was in, and what it had written on the side. Luckily, she got back to me rather fast, and said she’d found it and would leave it on the front counter. That place was on my way from dropping off the clothes on my trip going to Briarwood where we needed the music for the audience.
This group prepares food for us at the end of our music. Today was a great soup with tortellini, carrots, ground beef, cabbage, and was very tasty. Everyone loved it. They had good homemade croutons to add, Ritz crackers with cheese, and a wonderful orange Jello salad with mandarin oranges that went well with the hot soup. Also, there were cookies and a special crusty sweet pastry concoction, without fruit.
From there I went to Super 1 for John’s sausage contribution. He and the pruners are celebrating at the end of their last morning of pruning, this Monday. with tasty morsels, no doubt with wine. They have worked from 9 to Noon but will finish the short remaining rows by 11 – or not.
On to buy some gasoline for John’s car. Price has risen to $2.04. Then from there I went to drop off a bag of skirts (mostly) to our flute player. I had them at Briarwood, but she left in a hurry because the grandparents were visiting. I remembered her house address from when I was giving her directions to another friend’s house, and so it was right on my way home, and I stopped off and handed them to her. While I will see her tomorrow night, the time will be busy and involved with other things. Food and practice.
John fixed us a fabulous beef stew meat in the Crockpot with potatoes and mushrooms. I need to find out if eating as many mushrooms as we do is detrimental to my health. John just learned that they may contribute to high Uric acid. I was started a couple months ago on a pill to lower it, and while it has, some, my dosage was doubled this week by my Cardiologist.
Boy, I have been busy and I haven’t scanned for malware in 10 days. I have 3 programs I use faithfully, usually a couple times a week. But things have been so busy, I did not until tonight. [John says – Time to upgrade the operating system.]
Sunday, Mar 20
For Mar 19 CPAP. Reported figures, 7 hrs 55 min with AHI=2.63. Events: 19 H, 16 CSR, 2CA, 6 RERA. No major mask leaks (max=10 L/min); I haven’t done my oximeter yet.
Going to a potluck jam session tonight in prep for an upcoming performance. I need to finish Mountain Dew with corrected lyrics and chords added, and add a larger copy of T for Texas lyrics. John has put on a pork loin roast (he will add cherries from our trees to make a sauce for the side and add some baked Honeycrisp apples). We’ll potluck and practice afterwards for our performance April 2 at the Blue Agates Round and Square Dance Anniversary Dance dinner; they feed us and our spouses after we provide the dinner music. A dozen of us have played for them for several years. It is always a fun event. I think when April comes around, we may want to switch to that music for April for the Fiddlers & Friends group. Only problem will be I won’t have copies of all of the songs for our audiences. We will be able to pull a few from the books after the Irish songs. I’ll decide later.
Hope your week was fine.
Nancy and John
Still on the Naneum Fan